When thinking about and assessing population health, it’s important to consider all factors that can lead to adverse health outcomes and health system utilization patterns.
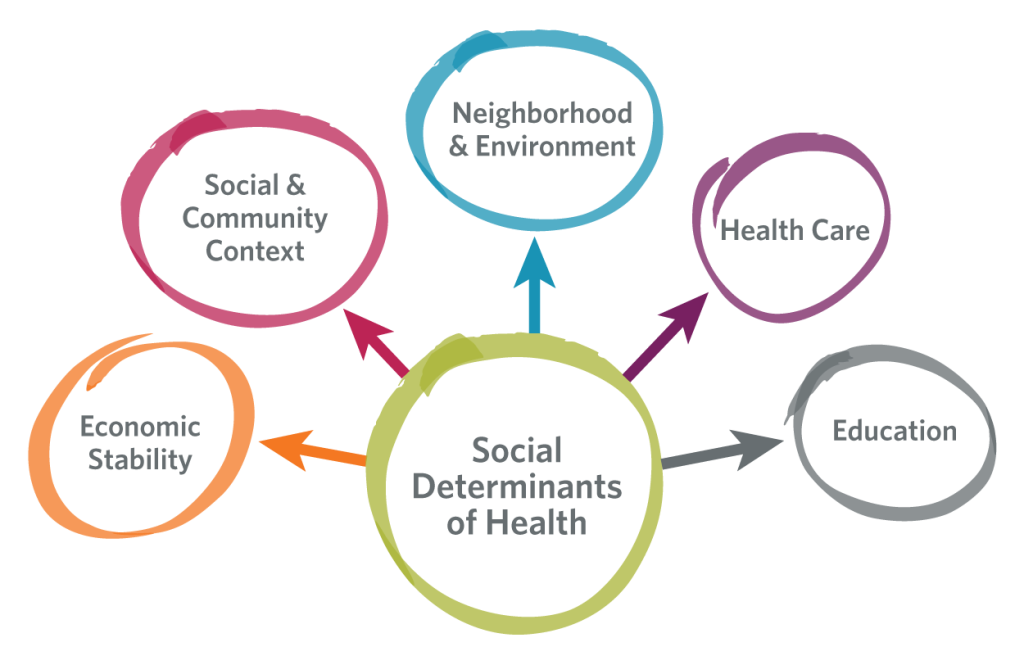
Social determinants of health (SDoH) are the conditions in which people live, including where they’re born, what they do for work, and how they age. These determinants range from economic risk, food insecurity, and unstable housing, to lack of access to transportation and unsafe neighborhoods – and they all impact the overall health of our population. A person’s ZIP code is a stronger predictor to their potential health outcomes than their genetic code (Graham, Ostrowski, Sabina, healthaffairs.com). These unaddressed patients’ social needs also can contribute to high costs for health systems and manifest in ways like readmissions and unexpected emergency department (ED) visits. Understanding and better addressing SDoH can help us gain insights into our patients and ultimately help us improve the overall quality of care that we provide.
For example, a 45-year-old man with previously well-controlled type 2 diabetes has recently been experiencing high blood sugar levels. Over the past 6 months, his A1C has increased. He readily admits to his provider that his medication adherence has worsened, and he has been more reliant on fast food. He attributes these changes to recent financial strain and an inability to afford his monthly medications and fresh food. He has less income from landscaping work in the winter months, and his utility bills have dramatically increased, largely due to costs of heating his poorly insulated home. (Dr. Thuy Bui, UPMC)
“These are real needs that, if unaddressed, create barriers to effective treatment and can lead to poor health outcomes,” said Minette Vaccariello, Product Manager at UPMC Enterprises. “As UPMC moves to value-based care delivery, like we are with our UPMC Children’s Hospital of Pittsburgh’s newly formed Pediatric Network, it is important for providers and their clinical teams to understand SDoH of their patients so that they can better manage their high-risk populations.”
Health systems across the country also are looking at SDoH. While some are just assessing analytics, others are building databases of community resources, and others are focusing on specific, actionable interventions. At UPMC Enterprises, we are working to connect analytic insights of our vulnerable populations with actionable SDoH interventions. Our team is working with operational champions, Tami Minnier and Dr. Rob Bart, as well as stakeholders at Children’s Hospital, to validate the analytics we’re uncovering. Additionally, we will be working with internal experts in this space to develop ways we can operationalize intervention strategies.
“The analytics are important, but identification isn’t enough,” said Vaccariello. “We need to understand the analytics in order to develop intervention strategies that can make a real impact on our vulnerable populations.”
UPMC is looking at two specific vulnerable populations: Medicare and Pediatric Medicaid. Clinical data is pulled from both of these populations and run through machine learning models in order to understand the correlation of these risk factors to identified outcomes. The patients and their spatial risk scores are then geospatially mapped in order to illustrate major pain points and to highlight where potential intervention strategies would have the most impact on patients and consequently value to UPMC.
“That hardest part is that this is a new space for hospital systems to tackle; providers and clinical teams have not had a way to access SDoH insights in a systematic way in the past,” continued Vaccariello. “There is very little tracking on SDoH intervention programs, specifically how addressing them can improve health outcomes, which makes tying this work back to ROI a challenge.”
Once these vulnerable populations are uncovered, the targeting strategy is next. What kind of outreach is going to be effective? How do we accomplish this outreach? What’s going to motivate this population? These are all questions that need to be carefully considered in order for the intervention to work.
“Our ultimate goal is to be able to analyze the data, identify a specific high-risk population, develop a targeted strategy to deploy, and then track this intervention to see what kind of impact it’s had on cost and reduction in utilization,” finished Vaccariello.
Social determinants of health play a major role in driving negative health outcomes and health system utilization patterns. By taking a hard look at SDoH and analyzing that data to create targeted intervention strategies, we can begin to track outcomes and begin to show how we can reduce the total cost of care for our high-risk, high-needs populations. Ultimately, this can help improve the way we deliver care.


